Brief
With Google and Wikipedia at our fingertips, many of us are more or less educated on common symptoms that accompany an illness, be it a simple cold or a minor heart attack, and are able to act immediately to counteract it. We also have the freedom to get over-the-counter medicines. You know, the funny thing is, we are so educated and think so highly of ourselves that for many of the usual sickness, we treat ourselves. Now, don’t get me wrong, a Paracetamol for fever or Ibuprofen for pain relief is common knowledge. What is alarming is that these and many other medicines can be gotten without any prescription.
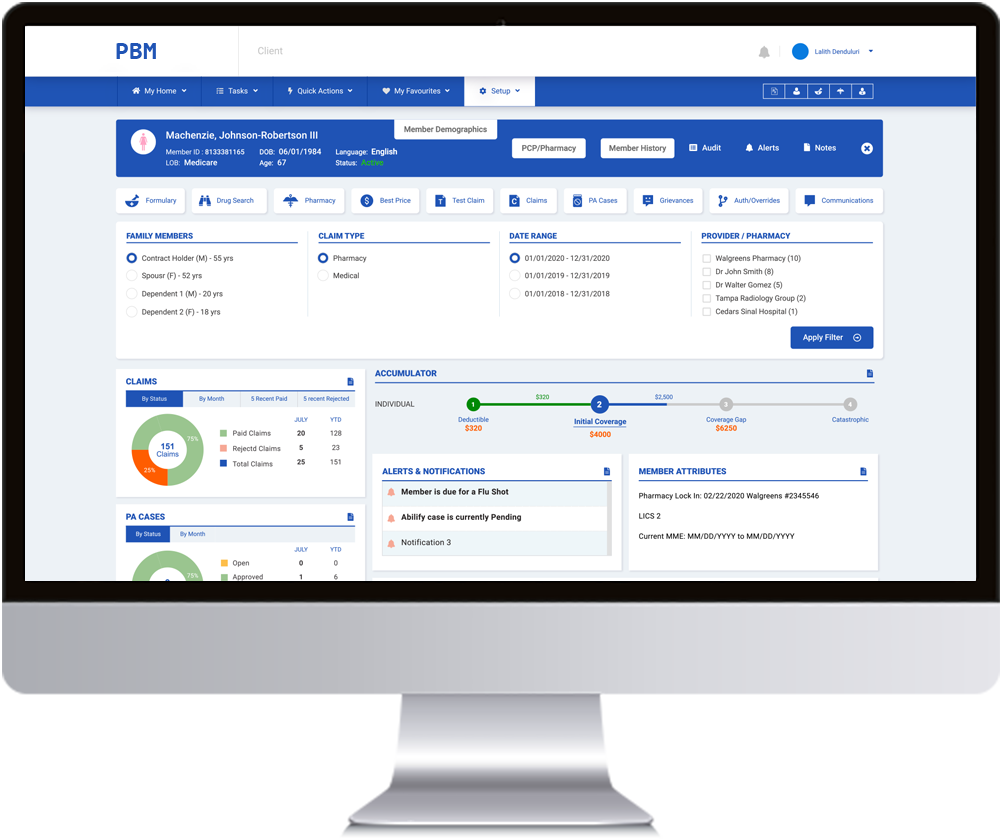
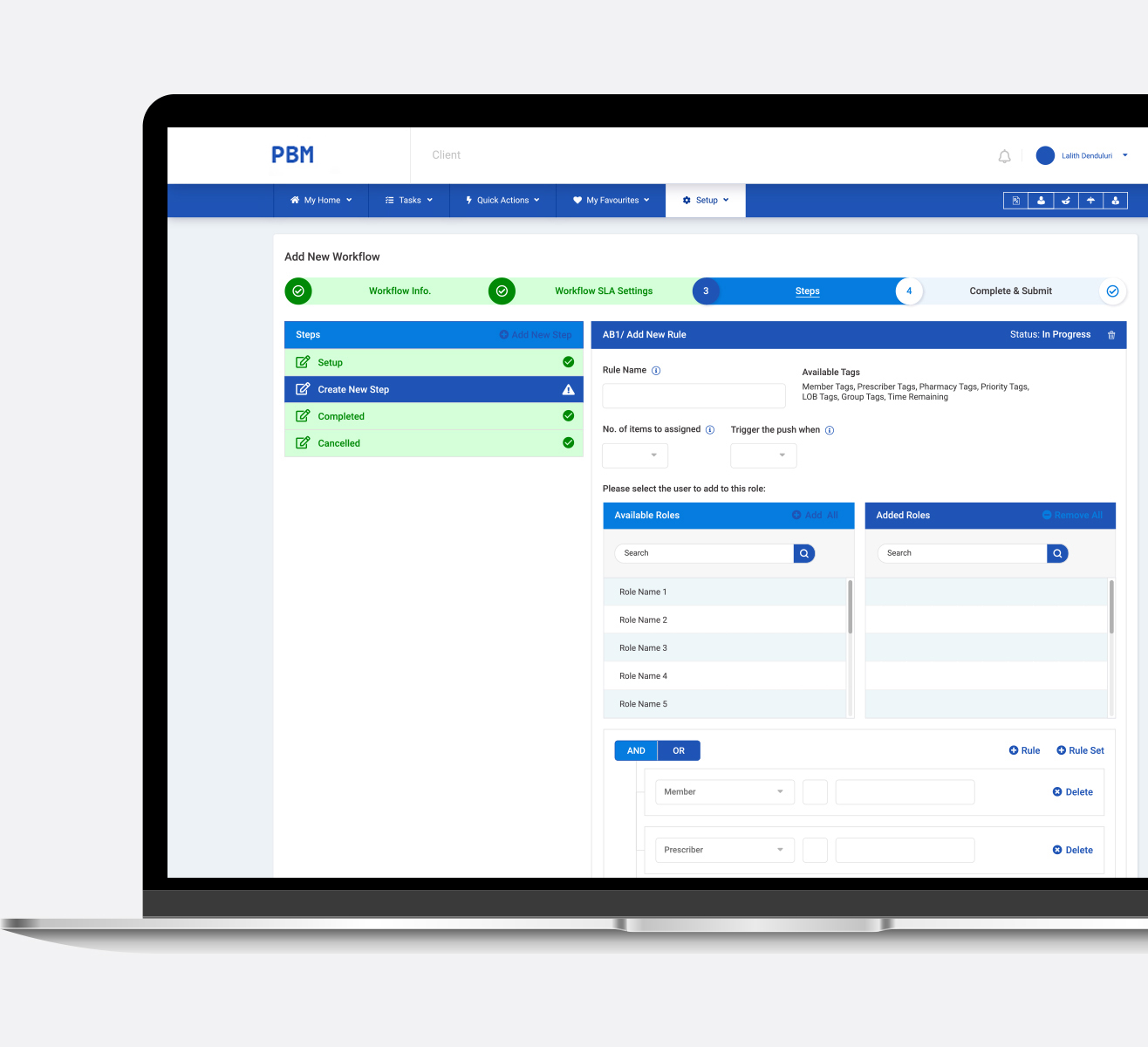
The US Healthcare industry has a group of “middlemen”, who are collectively known as PBMs – Pharmacy Benefit Managers. They have made use of the Prior Authorization Application (PA), a cost saving’s feature that helps ensure the appropriate use of selected prescription drugs. The working theory was pure and true to the cause, but, when it came to practice, many craved for the Midas Touch. What is it that we can do to take control of our lives, as well as, the life of our near and dear ones, back into our hands?
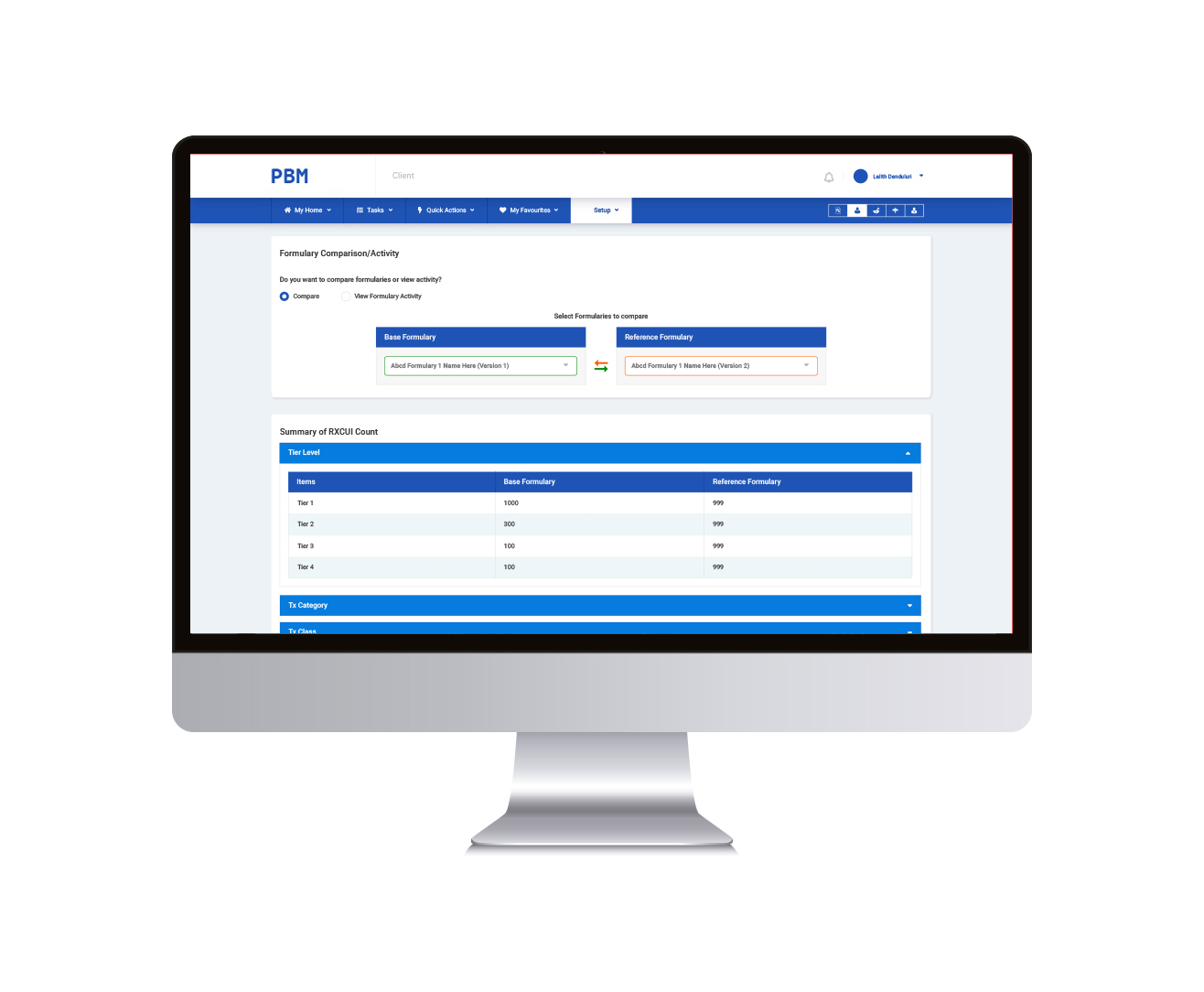
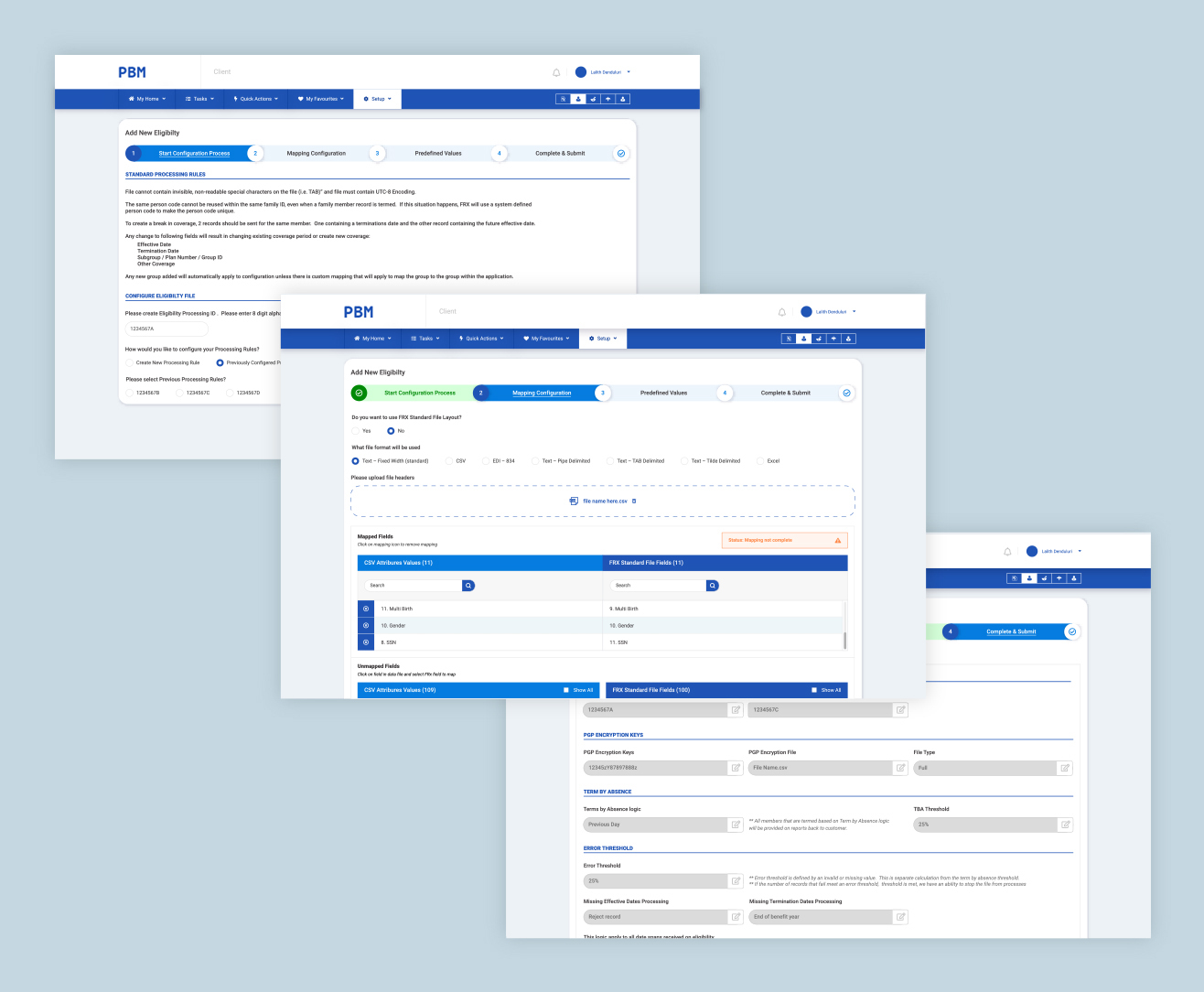
A leading enterprise in the healthcare industry proposed a solution – develop a software allowing you to reclaim control of your prescription drug benefit program, with cutting-edge technology that includes innovative administrative, operational and clinical services solutions. They approached us at Cloudium to bring this to fruition. PA is an automated process everywhere. So, what is different here? Our client wanted to bring about a change in how PBMs were perceived. That it is not just a cut throat business, it provides you with a feasible yet quality care.